Back pain: the consequence of a sedentary society
A healthy back for a happy life
Did you know that back pain is the number one reason for long-term incapacity for work? However, a patient’s expectations affect the recovery process and therefore the duration of their absence from work. According to a study in the Australian Journal of Physiotherapy, patients suffering from non-specific back pain with a positive attitude to the recovery process recovered twice as fast as those with negative expectations. Dr Peter Gartner, Medical Director at Park Igls, puts the blame on our sedentary society. ‘Our ancestor, Homo erectus – the first to walk upright – was very similar to us anatomically, and the perfect endurance runner. Not much has changed since then, at least from an anatomical standpoint.’ Dr Gartner explains: ‘Our entire body, from the skeleton to the muscles, is designed to move when upright.’ Human bodies are supposed to move!
Homo sedens
Physiotherapists Lisa French and Mina Siehs agree: ‘Looking at modern society, it is clear that we have metamorphosed from Homo erectus who moves, to Homo sedens who sits. Motionless. It’s not physically strenuous, so why do we still feel the strain? All too often, we carry heavy physical and mental loads which put pressure on the spine, intervertebral discs, cartilage and joints.’ The results are many and can be very painful. ‘They say sitting is the new smoking. Slumping in a chair doesn’t necessarily cause lasting damage, but sitting stationary for long periods of time is not recommended. Healthy sitting is about change: remember, the next position is the best one. The spine needs constant movement – strain and relief – to stay healthy, and frequently changing position helps achieve this.’
The importance of movement is becoming increasingly evident in both therapeutic intervention and prevention. In fact, without movement, everything really does come to a stop. ‘Too little physical activity can significantly affect muscle tension imbalances and therefore cause pain,’ Lisa French explains.

Back trouble
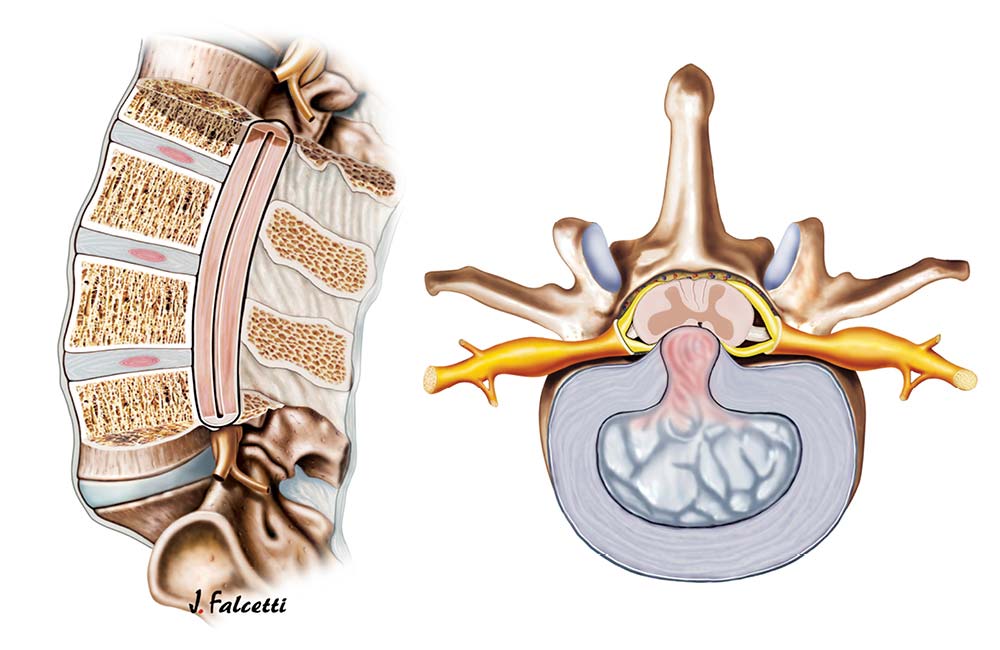
Back pain is now society’s number one common ailment. Slipped or herniated discs are often to blame, and, in fact, MRI scans have already detected precisely this problem in a third of young adults in Austria. But not all cases necessarily cause pain. ‘Pain arises when the pressure of a slipped disc causes inflammation and swelling, irritating the nerves. Typical symptoms include pain that spreads to the limbs, numbness or signs of paralysis,’ explains Dr Gartner. There are many causes for slipped discs, ranging from connective tissue weakness, malformation, poor posture and strain, to bending or twisting the wrong way.
‘The intervertebral discs need constant strain and release to ensure long term functionality. Uneven strain over long periods can affect disc structure, making them more prone to injury. It is important to regularly activate the girdle of muscles that supports our spine, allowing pressure to be evenly distributed and giving all tissue a healthy share of the strain. Uneven strain and lack of muscle movement can overload the discs in the long run. And when we’re in pain, we respond by adopting an unhelpful protective posture… it’s a vicious circle!’ Mina Siehs highlights.
Note:
Discs function as both shock absorbers and as a link between the vertebrae of our spine. We have 23 spinal discs, consisting of a tougher outer casing and jelly-like centre. A herniated disc (prolapse) occurs when some of the softer jelly escapes through a tear in the outer casing. A protrusion, on the other hand, is when the disc bulges to the front and the outer cartilage remains intact.


Holistic diagnosis
‘Broadly speaking, we differentiate between two types of back pain in diagnosis: specific and non-specific back pain,’ Dr Gartner explains. ‘The first has a specific anatomic, traumatic or pathological cause like an abnormality, accident or inflammatory disease, for example a kidney inflammation or ankylosing spondylitis, while non-specific back pain cannot be ascribed to a concrete cause. So each patient and their particular situation must be examined as a whole,’ he stresses.
While physical factors play a major role, pain is a complex process. Psychological and sociocultural circumstances can also influence the perception of pain. ‘Stress hormones lead to muscle tension that can in turn result in pain. Depression changes the perception of pain and can increase fear of pain, which alters posture and movement significantly. This often results in avoiding particular movements, which then leads to muscle weakness, tension and poor posture. The perception of pain is also altered by an increased focus on pain or fixating on worst-case scenarios.’ Dr Gartner explains: ‘Every chronic pain diagnosis and therapy plan should incorporate a psycho-social approach.’

Holistic therapy
Treating back pain with sprays and infusion therapy isn’t necessarily the answer. ‘Infusion therapy and sprays can and do provide relief, but they cannot treat the causes,’ Dr Gartner warns. ‘In most cases, non-specific pain returns.’ The winning combination is pain therapy with physiotherapy, psychotherapy and lifestyle changes. Exercise therapy is also effective, and, according to physiotherapist Mina Siehs: ‘the type of exercise is best decided between doctor and patient on a case-by-case basis.’ There are a number of good options. For example, fascia training is becoming popular. ‘Fascia therapies like massage, rollers or stretches have an immediate effect on the nervous system which causes the tissues to relax. However, the effect doesn’t usually last long.’ Other active strategies include movement training and strength training which increase resilience (due to physiological changes in the tissue) and encourage the patient to carry on independently. It also gives them a push to tackle their symptoms over the long term.
‘At Park Igls we use our knowledge of the Feldenkrais® Method to help patients relearn patterns of movement. Yoga exercises increase range of motion. The revolutionary kybun® or trampoline training – which is gentle on joints – stabilises the core and back muscles. Running and walking – virtually the most natural forms of movement – are also important. Of course what’s more important is that the movement is performed correctly,’ Mina Siehs explains. Dr Gartner highlights: ‘Exercise is absolutely fundamental in all cases. Back pain simply won’t improve without it.’
Note:
Park Igls offers almost 50 different types of exercise. The medical team takes patients’ individual preferences and requirements into consideration, but the therapists agree that the most important thing is that the chosen exercise is fun, otherwise you’d never keep it up!
Photo credits: Park Igls, iStock
If this story has got you interested in starting your journey with Niche Destinations, please enquire here.
A WORLD OF STORIES
If this story has got you interested in starting your journey with Niche Destinations, please enquire here.